Healthier Together – Improving the Quality of Care for Children and Young People in Wessex
The Healthier Together Programme is developed in partnership with parents and healthcare professionals across Dorset, Hampshire and Isle of Wight.
The Problem
In the UK, emergency paediatric admissions rose by 13% between 2013-2017. The workforce across primary, emergency and paediatric care have to meet the ongoing health needs of the population, and digital solutions such as web-based resources with single point of access can improve care (Topol Report 2019).
Inconsistent messages from healthcare professionals generate anxiety for parents and impacts on subsequent health-seeking behaviour. The Healthier Together programme was established in Wessex in 2014 to promote integrated working across health and social care to ensure consistency across the urgent care pathway and provide access to high quality resources promoting self-care for families.
Aims
Core Principles:
- Parents feel empowered about whether and when to seek the advice of a healthcare professional.
- Parents are clearly signposted to appropriate healthcare services when required.
- Parents should receive consistent and appropriate advice across the whole urgent care system.
- At every point of contact, the healthcare practitioner has a clear understanding of the limits of their own competence and when and where to seek guidance.
- Local referral pathways and clinical guidelines across the whole acute care system are standardised and understood by all healthcare practitioners.
- Effective communication and information sharing between healthcare practitioners and services across the whole acute care system should be in place.
Making the Case For Change
Digital technologies are transforming the ability to empower patients and their families/carers to participate actively in their own care, with a greater focus on well-being. Analysis in Hampshire of parents’ perceptions found their worries around health needs in their children reduced by access to the Healthier Together digital resources and that they expect their health seeking behaviour to change with continuing access to the digital strategy.
The Healthier Together website provides clear information on common childhood illnesses used by both families and healthcare professionals, including advice on what ‘red-flag’ signs to look out for, where to seek help if required, what they should do to keep their child comfortable and how long their child’s symptoms are likely to last.
Co-design has been a crucial aspect of the success of the programme. From the outset, views of parents and carers were sought, along with those of the healthcare professionals delivering urgent care paediatric services. Relationship building across organisational boundaries has enabled the production of clinical resources and agreement on treatment pathways and safety netting resources. In addition, an extensive education programme involving all professional groups involved in the care of children has been the catalyst for successful implementation.

Our Improvement
The programme has been a driver for service improvement across Wessex, including the roll-out of connecting care children’s hubs, piloting of a paediatric desk within NHS 111, trialling of a digital app for parents promoting self-care for minor illnesses, improving antibiotic prescribing in primary care, delivering education on mental health and wellbeing to primary school children and evaluating the impact of social prescribing (minor illness workshops) for parents. In addition, national resources have been developed in partnership with the RCPCH, RCGP and Institute of Health Visiting to support parents during the COVID-19 pandemic.
The Fontanelle podcasts have also been produced for clinicians with a version for families currently in development.
Graph 1 (below), shows the quarterly usage of the Healthier Together website:
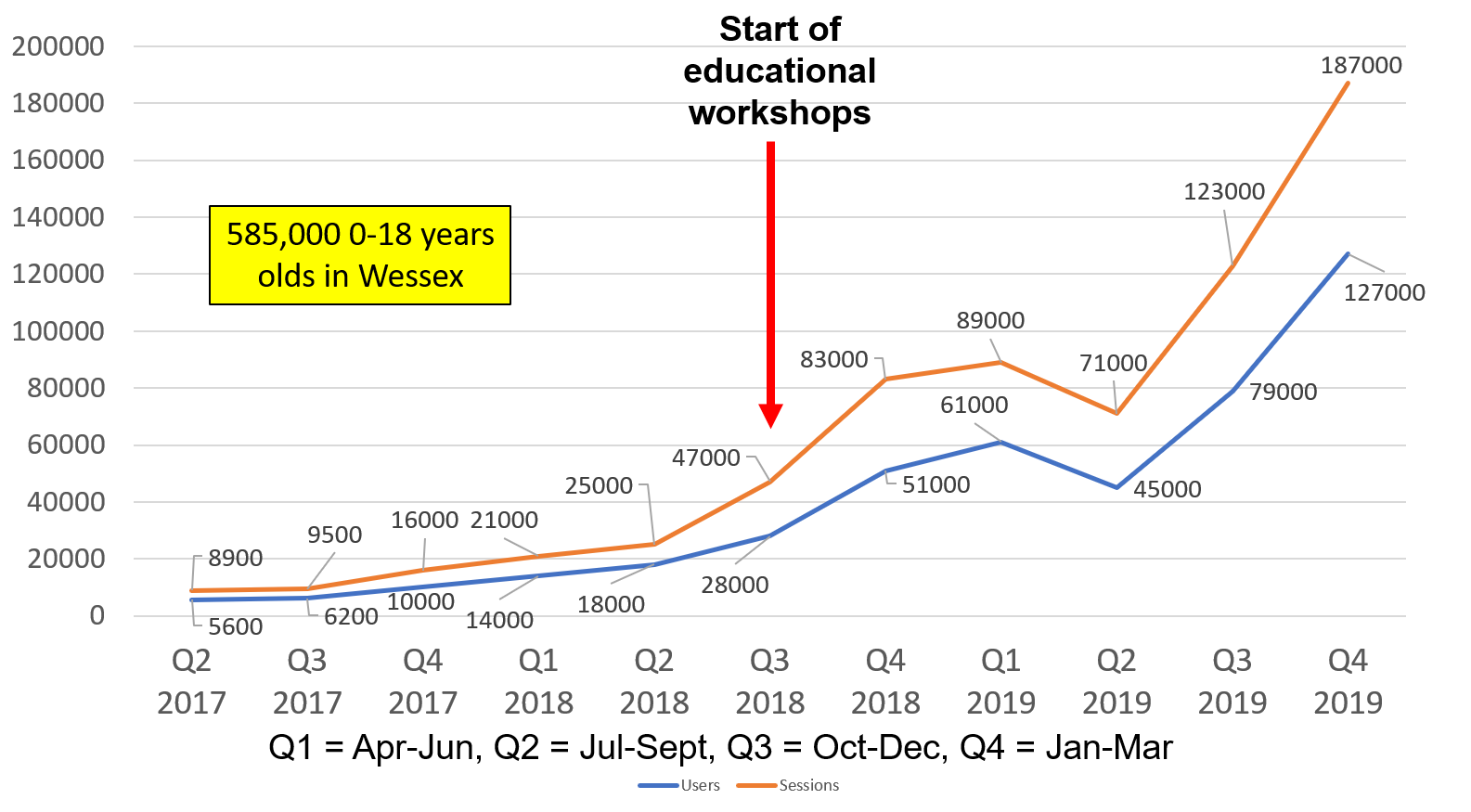
Graph 2 (below), shows the impact on emergency admissions (aged 0-18 years) following the introduction of the Healthier Together website and parent education sessions in Hampshire:
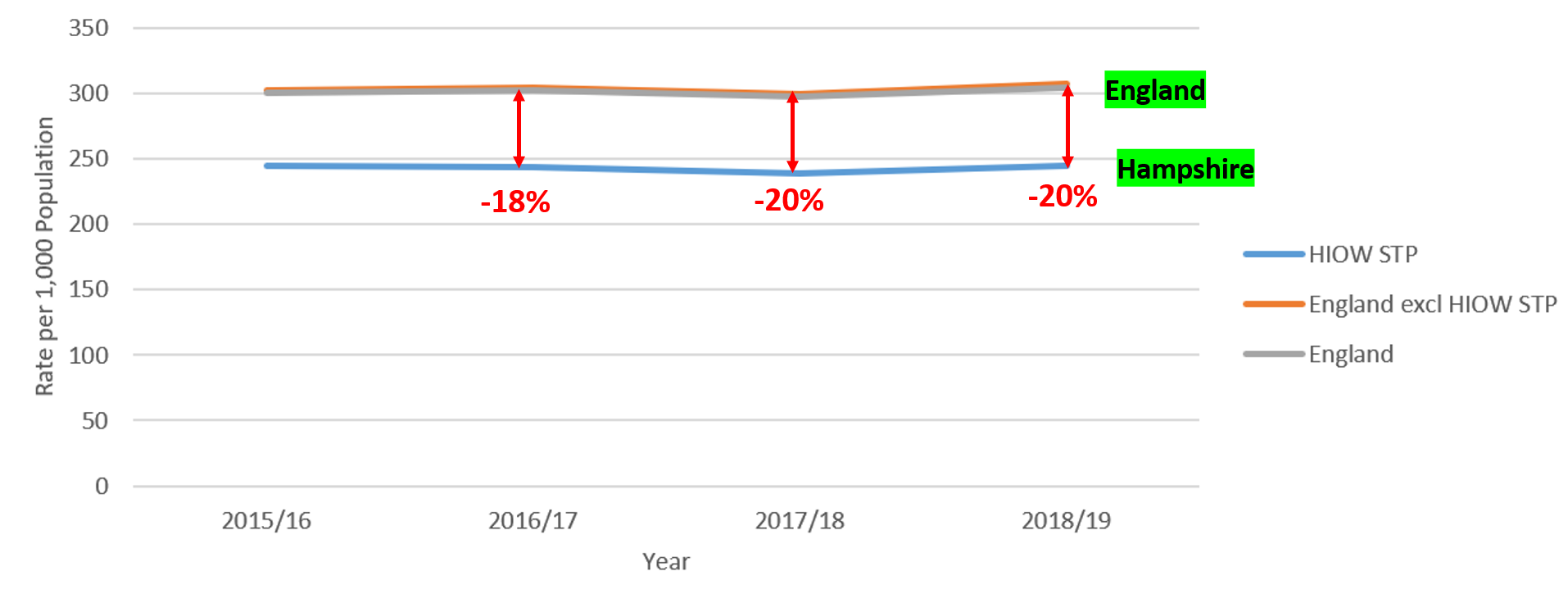
Graph 3 (below), shows the impact of the Healthier Together website and parent education sessions in Hampshire on reduced GP appointments:
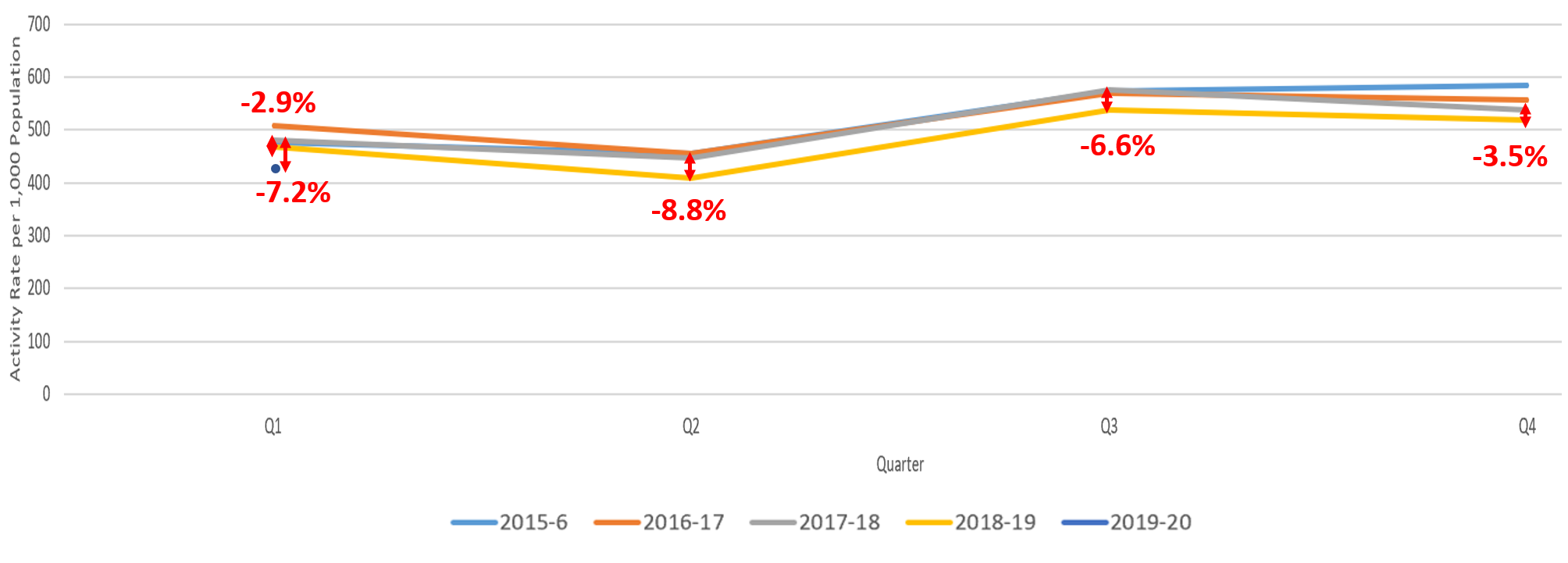
Graph 4 (below), shows the impact of the Healthier Together website and parent education sessions on antibiotic prescriptions for children aged 0-18 years in Hampshire:

Learning and Next Steps
Formal evaluation of the programme was conducted by University of Winchester.
Feedback from parents includes:
“We’ve been through a month or more of our child being ill with several virus infections and a number of visits to the doctors. It’s been a very stressful and worrying time. I’ve just come across this website and it’s BRILLIANT. Simple, reassuring and helpful. THANK YOU.”
“It’s like a mini doctor for you at home, that’s how I see it. It gives all information, what should I do, in what cases I need to go to hospital or how I can treat my baby at home.”
The success of the Healthier Together programme relies upon dedicated clinical leadership to drive engagement from local clinicians; co-design and collaboration is paramount. For this reason, such a programme requires local implementation rather than national roll-out. The Healthier Together website is free for others to take in part/whole and adapt for local use; a number of STPs/health boards are in the process of doing so.
The Healthier Together website was presented at RCPCH Annual Conference and the NHS Health and Care Innovation Expo in 2019. A copy of the full presentation slide deck can be found below.
Visit the Healthier Together website.
Project Lead: Dr Sanjay Patel, Consultant Paediatrician, Southampton Children’s Hospital
Organisation: Healthier Together Programme, Wessex
Published: June 2020
